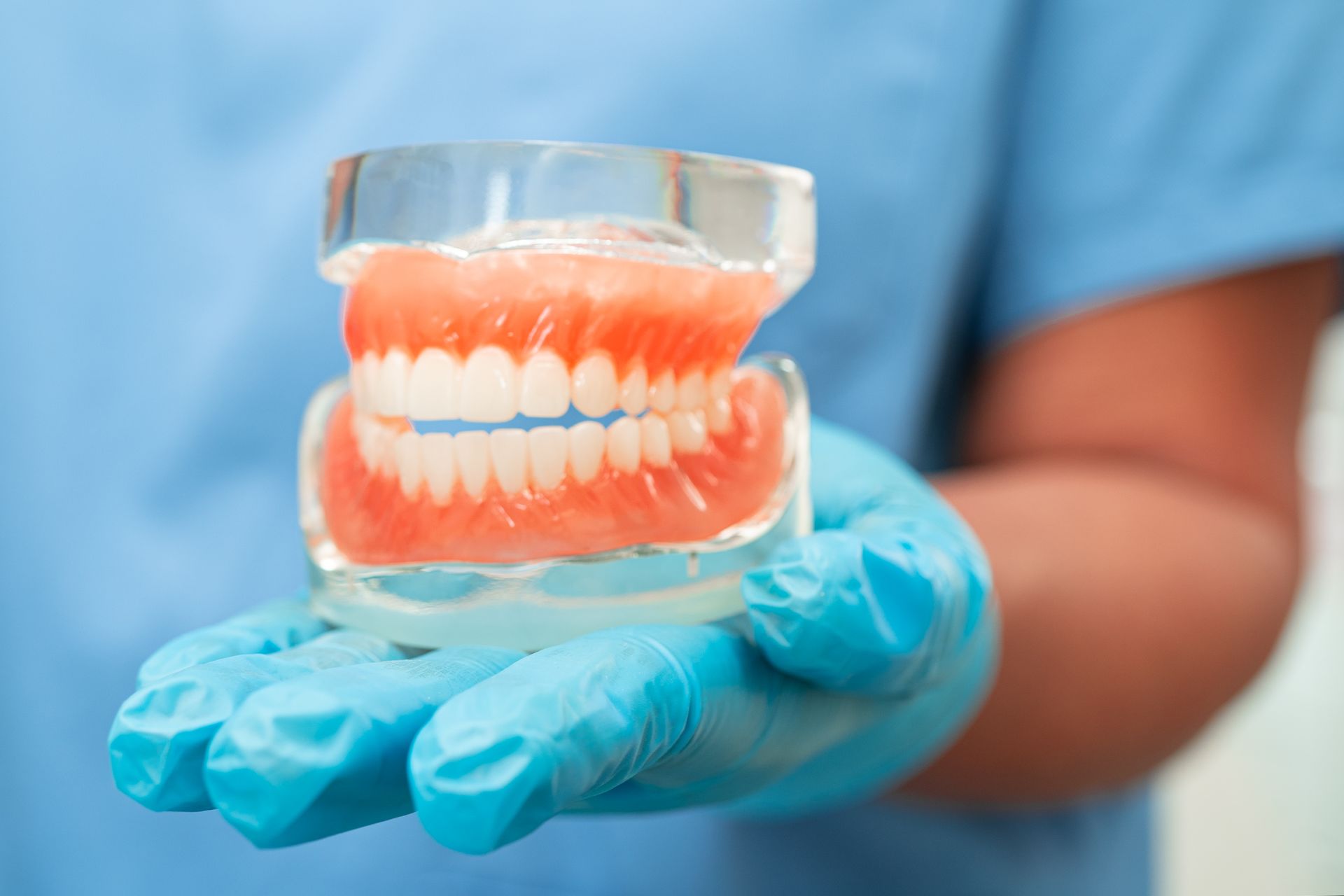
Bottom Dentures and Implants: How 2–4 Implants Can Stabilize Your Lower Denture
At Innate Dental Solutions, our clinical team plans and restores implant-retained overdentures and fixed implant bridges as part of everyday care. We see what makes lower dentures slip, what actually improves stability, and what patients need to know before choosing 2 implants, 4 implants, or a fixed option. This guide is written to be clear and practical, based on real treatment planning and long-term maintenance needs.
Introduction: Why Lower Dentures Move So Much (and what implants change)
Lower dentures move for one main reason: there isn't much holding them down. The lower jaw has less surface area than the upper jaw, and your tongue and cheeks push on the denture all day. Even a well-made lower denture can rock, lift, or slide.
Dental implants change the problem. Instead of relying only on gums and suction, the denture can connect to implant posts in the jawbone. That connection is what creates real denture retention and stability.
The day-to-day problems people notice (slipping, sore spots, eating, speech, confidence)
When a lower denture is loose, people often deal with:
- Denture slipping when talking or laughing
- Clicking or rocking during meals
- Sore spots, gum irritation, and frequent adjustments
- Trouble chewing tougher foods (meat, salad, crusty bread)
- Worry about the denture moving in public
If any of this sounds familiar, implants are one of the most reliable ways to steady the lower denture. If you're still weighing your options, our guide on dentures vs. dental implants breaks down the key differences to help you decide.
Why Bottom Dentures Are Harder to Keep in Place Than Top Dentures
Upper dentures can sometimes "seal" to the palate and use suction. Lower dentures can't. The lower denture sits on a smaller ridge of bone, and it has to share space with the tongue, the floor of the mouth, and strong cheek muscles.
Lower jaw anatomy and soft-tissue forces (tongue, cheeks, ridge shape)
The lower denture is constantly fighting movement. Your tongue pushes outward. Your cheeks push inward. The ridge of bone under the denture can also shrink over time, which makes the denture fit looser. This is why a lower denture that once felt "okay" can slowly become harder to control.
Why suction/adhesives don't reliably solve the problem long-term
Adhesives can help short-term, but they do not stop the denture from rocking under pressure. They also don't prevent the bone under the denture from shrinking over time. Many people end up using more and more adhesive just to get through meals.
Implants are different because they add firm anchor points in the jawbone. That reduces sliding and rocking in a way adhesives usually can't.
How Dental Implants Stabilize a Lower Denture
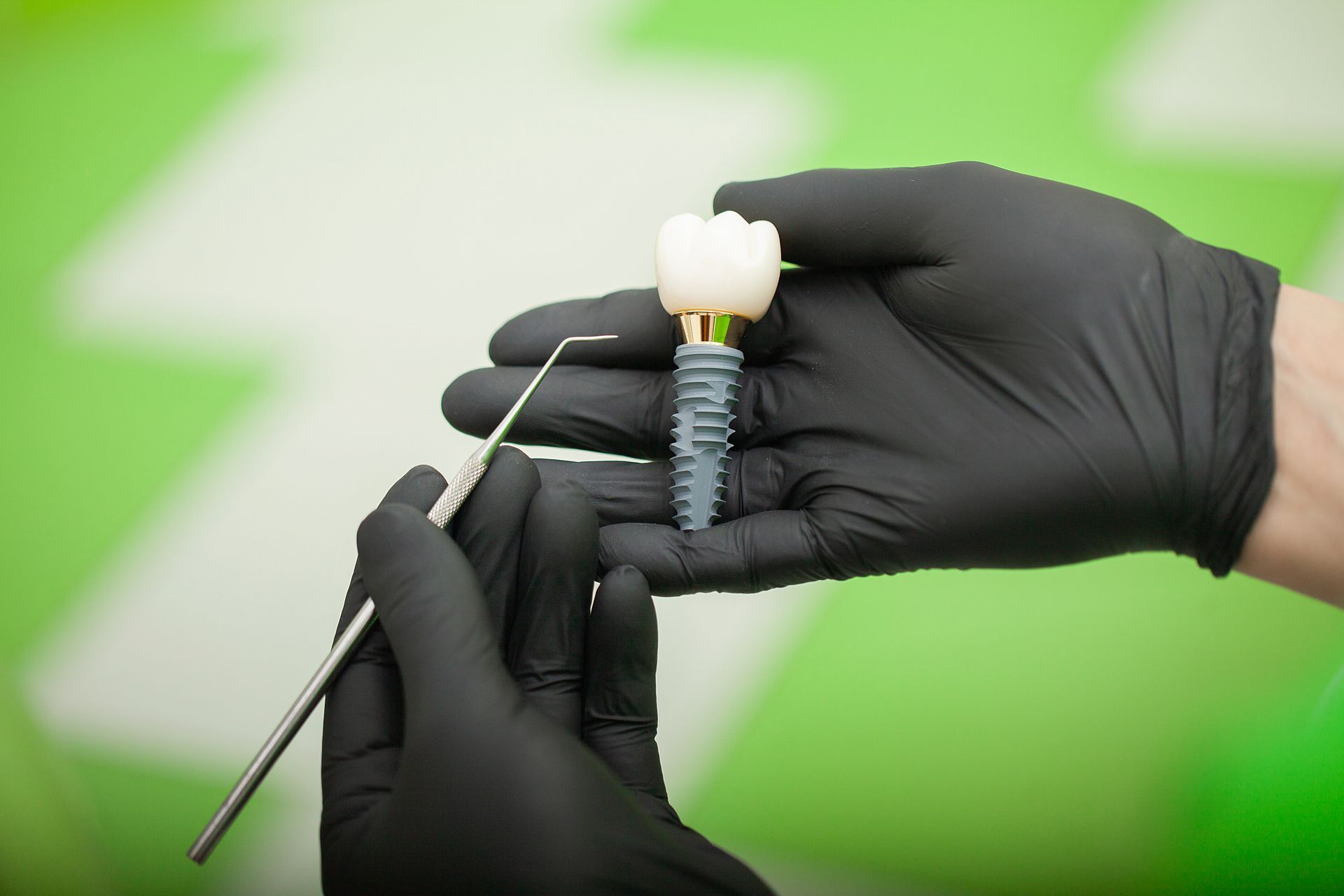
Implants act like small roots made of titanium. They sit in the jawbone and support attachment parts that connect to a denture. This can turn a loose lower denture into a stable, confident fit.
Osseointegration in plain language (how implants "lock in")
After an implant is placed, the bone heals tightly around it. This is called osseointegration. In simple terms, the implant becomes part of the bone. Once it is stable, it can hold an attachment or support a fixed bridge.
"Implant-retained" vs "implant-supported" (what those terms mean clinically)
These terms sound similar, but they can mean different things:
Implant-retained denture - The implants mainly provide "hold." The denture still rests on the gums, but it snaps onto implants so it doesn't lift or slide easily.
Implant-supported denture - The implants take more of the chewing force. Depending on the design (like a bar-retained overdenture or a fixed bridge), the gums may carry less load. Many patients feel this as a steadier bite and less rocking.
For a deeper look at how an implant goes from consultation to crown, see our overview of how a dental implant is inserted.
Your Main Options for Implant-Stabilized Bottom Dentures
There isn't one best choice for everyone. The right fit depends on your goals, your bone, your bite, and how you want to clean your teeth.
Implant-retained overdenture (snap-in / removable)
This is often called "snap-in dentures" or "snap-on lower denture implants." The denture is removable at home, but it connects to the implants using small attachments. Learn more about snap-on dental implants and whether this design fits your lifestyle.
Common reasons people choose a snap-in overdenture:
- Big improvement in stability with a removable design
- Easier cleaning (you remove it to brush and rinse)
- Often a simpler and more affordable path than fixed teeth
Fixed, screw-retained denture (hybrid bridge / non-removable at home)
This option is sometimes called a fixed implant denture, fixed screw-retained denture, or hybrid bridge. You do not take it out at home. Your dentist removes it for maintenance visits.
Common reasons people choose fixed teeth:
- The most "locked-in" feel
- Strong chewing power and less movement
- Feels closer to natural teeth for many patients
This option usually needs more implants and careful planning to handle bite forces. If you're comparing this path to a removable option, our snap-in dentures vs. All-on-4 guide is a helpful starting point.
Mini dental implants (when they may be considered)
Mini dental implants are narrower implants. They can be considered in certain cases, especially when bone volume is limited or when a patient needs a less invasive approach. They are not the best choice for every bite or every bone type, and long-term durability depends on the case. A full exam and imaging matter here.
How Many Implants Do You Need for a Lower Denture: 2 vs 4
Here's the straight answer up front:
- Two implants can greatly improve denture retention and reduce lifting.
- Four implants usually feels more stable, with less rocking, and can support stronger designs.
The "right" number depends on what you want the denture to do.
When two implants may be enough (basic retention, simpler maintenance)
Two implants are often placed in the front part of the lower jaw, where bone is commonly stronger. This setup can:
- Reduce slipping and lifting
- Cut down on sore spots caused by denture movement
- Make eating and speaking easier
Two implants can be a great step up from a traditional lower denture, especially if your main goal is to stop it from popping up or sliding around.
When four implants are recommended (more stability, less rocking, stronger bite)
Four implants usually spread support across a wider area. This often leads to:
- Less rocking during chewing
- More confidence with tougher foods
- A more secure feel, especially if your denture has been unstable for years
Four implants can also give more options for attachment systems, including bar designs that can feel very stable.
When four or more may be advised (fixed options, higher bite forces, bone conditions)
If you want a fixed bridge (non-removable at home), most cases need more implant support than a simple snap-in. Higher bite forces, grinding, and bone conditions can also push the plan toward more implants and stronger materials. Our All-on-4 implants page covers what a four-implant fixed solution looks like in practice.
Key factors that determine implant count (bone volume/quality, anatomy, goals, budget)
A good treatment plan looks at:
- Bone density and volume (and where the best bone is)
- Jaw shape and nerve positions
- Your bite forces and chewing habits
- Whether you want removable or fixed teeth
- Your budget and whether phased treatment makes sense
Attachment Systems and Implant Configurations That Affect "How It Feels"
Two people can both have "lower denture implants" and have very different experiences. Often, the difference is the attachment system.
Stud/Locator-style attachments (what "snap" retention is)
Locator-style attachments are common for implant-retained overdentures. The denture snaps onto the implants using small inserts (often nylon inserts). Many patients like them because the denture feels secure, but it's still easy to remove for cleaning. Over time, inserts can wear down. That's normal. Replacing them is one of the main ways retention is refreshed.
Ball/O-ring attachments
Ball attachments use an O-ring to hold the denture in place. They can work well and are a known option for snap-in dentures. Like other systems, parts can wear and need replacement.
Bar-retained overdentures (splinting implants for added stability)
A bar-retained overdenture connects implants with a thin metal bar. The denture clips onto the bar. This can spread force across implants, improve stability, and reduce rocking. It works well when four implants are used. Bars can feel very solid, but cleaning takes a bit more effort because you need to clean around the bar daily.
Wear items and maintenance (inserts/clips and how retention is refreshed)
No attachment system is "set it and forget it." Most overdentures need insert or clip replacement as parts wear, periodic relines as gum shape changes, and routine checks to protect implants and fit. This is normal maintenance, similar to how tires wear on a car. Our dental implant maintenance page outlines what to expect long-term.
Benefits of Bottom Denture Implants (What Improves First)
Most people notice improvements quickly once the denture connects securely.
Eating and chewing efficiency
A stable denture helps you bite and chew with more confidence. Many people find they can eat a wider range of foods because the denture is not sliding around.
Speech and comfort (less movement = fewer sore spots)
When a denture moves less, the gums get less rubbing. That often means fewer sore spots and less gum irritation. Speech can also feel easier when the denture isn't lifting or clicking.
Adhesive-free stability
Many implant overdenture patients reduce or stop using denture adhesive. That alone can be a huge quality-of-life upgrade.
Bone preservation support over time
When implants are in the jawbone, they can help maintain bone in those areas by providing functional stimulation. While bone changes can still happen, implants often offer better long-term support than a denture sitting on the gums alone. If you're concerned about bone loss affecting your candidacy, see whether you can get dental implants if you have bone loss.
What the Treatment Process Looks Like
Most plans follow a clear sequence, even if the timing differs by patient.
Consultation, exam, and 3D imaging/planning
This is where candidacy is confirmed. Your dentist checks bone volume and density, gum health, bite and jaw relationships, and space needed for a strong denture design. 3D imaging helps plan safe, accurate implant placement.
Implant placement visit
Implants are placed in the jawbone. Some cases also include extractions or bone augmentation, depending on what you start with. If bone augmentation is part of your plan, learn more about what bone grafting for dental implants involves.
Healing and osseointegration timeline
Healing is when the bone locks onto the implant. The timeline varies by person and by bone quality. During this phase, your denture plan may involve a temporary solution or modifications to your current denture.
Connecting the denture (snap attachments, bar, or fixed bridge)
Once implants are ready, the attachment parts are placed and the denture is fitted to connect securely. This is often the moment patients feel the biggest change in stability.
Bite and speech refinement (adjustments that make it feel "right")
Even a stable denture may need small adjustments to feel natural. Your dentist fine-tunes the bite and comfort, especially in the first weeks.
Who's a Good Candidate (and What Can Change the Plan)
Many people with loose lower dentures can qualify, but the details matter. If you've wondered whether someone with no remaining teeth can still pursue implants, the answer is often yes, see whether you can get dental implants if you have no teeth.
Bone density/volume and when grafting or angled strategies are considered
If bone is thin or low in certain areas, your dentist may discuss bone augmentation or different implant positioning. Good planning focuses on placing implants where they can be stable and protected.
Health factors (uncontrolled conditions, smoking)
Some medical conditions and smoking can slow healing and raise risks. This doesn't always mean "no," but it may change timing, steps, or the type of restoration recommended.
Bite forces and habits (clenching/grinding)
Strong bite forces and grinding can stress implants and attachments. In these cases, the plan may lean toward more support, stronger materials, and sometimes a night guard.
When mini implants or alternative configurations might fit
If standard implants are not ideal, mini implants or other configurations may be considered. The best choice depends on stability needs and long-term goals.
Care and Maintenance: Removable vs Fixed
Long-term success depends on daily care.
Daily cleaning routine for snap-in overdentures
Most patients do best with a simple routine:
- Remove the denture to brush it
- Clean around the implant attachments
- Rinse and inspect for buildup
Your dentist may recommend tools like soft brushes or water flossers to keep attachments clean.
Daily cleaning routine for fixed bridges (under-bridge hygiene tools)
Fixed teeth require cleaning underneath the bridge. Common tools include super-floss or floss threaders, interdental brushes, and water flossers. It's not hard, but it must be done consistently.
Professional maintenance schedule (checks, insert replacement, periodic deep cleaning)
Plan on regular visits to check implant health, refresh worn inserts or clips, adjust fit as your mouth changes, and deep clean around fixed bridges.
Realistic Trade-Offs to Understand Before You Decide
Implants can be life-changing, but it helps to be honest about the downsides.
Surgery and healing time
Implants are a surgical procedure. There is healing time, and some soreness is normal. Most people do well, but you should expect a recovery period.
Hygiene commitment and long-term upkeep
Implants need daily cleaning. Attachments wear. Dentures may need relines. This is normal maintenance, but it's part of the deal.
Cost considerations vs quality-of-life gains
Implants are an investment. For a full breakdown of what drives pricing, visit our cost of dental implants page. The plan should match what you can maintain long-term.
Cost and Insurance Factors (What Typically Changes the Price)
Prices vary widely because the plan varies widely.
Implant number/type, denture type, needed add-on procedures
Common cost drivers include:
- Two implants vs four implants (or more)
- Removable overdenture vs fixed screw-retained bridge
- Attachment type (stud vs bar)
- Extractions, bone augmentation, or other prep work
- Materials used for the denture/bridge
Financing or phased-treatment approaches to discuss
Some people start with a simpler plan (like two implants and a snap-in overdenture) and upgrade later. In other cases, it makes sense to do it all at once. A clear treatment plan helps you compare options.
Conclusion: Choosing the Right Stability Level for Your Lifestyle
If your lower denture slips, hurts, or makes eating stressful, implants can make a real difference. Two implants can be a strong starting point for better retention. Four implants often provide a steadier feel and more design options, especially if rocking has been a big problem.
Summary of who tends to do best with 2 implants vs 4 implants
Two implants often fit best for people who want a simpler removable denture with solid "snap" retention. Four implants often fit best for people who want stronger stability, less rocking, and more support for higher bite forces or bar designs.
Schedule an implant evaluation and get a personalized plan
The best next step is a proper exam with 3D imaging and a clear discussion of your goals. That's how you find out what your bone allows, what level of stability is realistic, and which option you can comfortably maintain for years. Contact Innate Dental Solutions to schedule your evaluation.